A student stands over a patient, needle poised. They have a “perfect” prescription: a textbook combination of points harvested from a lecture slide on chronic lower back pain. But as the needle meets the skin, the student hesitates - the symptom of a quiet habit that has taken hold of our profession. We routinely say we “prescribe” points. It sounds efficient. It echoes the authority of biomedical culture and fits neatly into the insurance field. But vocabulary is never neutral; repeated long enough, it dictates behavior.
Integrative Tui Na for TMJD
It is not uncommon for a patient to come into the office of an acupuncturist complaining of a history of jaw pain, stress and headaches, with a diagnosis of temporal mandibular joint dysfunction (TMJD). This can present itself many ways, usually consisting of pain, bruxism (teeth grinding), crepitus (popping/cracking), and decreased range of motion. From a Chinese medical perspective it can fit into an array of patterns. In my practice, the most common differentiation I see is liver xue deficiency, qi stagnation or stomach heat, although they are not the only patterns that can arise. Treating these underlying patterns is essential but for immediate pain relief, I utilize the techniques of Integrative tui na.
The first step in assessing a patient with TMJD is to visualize the opening and closing of the mouth and palpate the mandible during this action. The visualization can show if there is any deviation of the jaw, providing an excellent idea as to which side more muscular tension is present. The palpation is useful to assess the alignment of the temporal mandibular joint. When assessing a patient with TMJD, I also pay careful attention to their posture and joint play, especially in the cervical region. When a patient has an abnormal lordotic curve (anterior head carriage), decreased joint play or decreased range of motion in the cervical region, it can exacerbate or be an underlying cause of TMJD. If the cervical spine is not in alignment, the head will not be aligned either, leading to or exacerbating jaw pain.
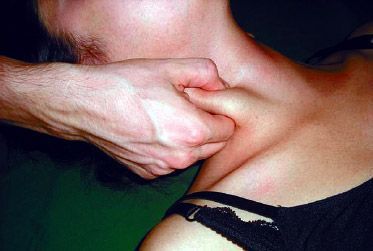
Taking into consideration the results of assessment the treatment can continue. I often perform tui na for TMJD after needling so the patient is relaxed, thereby allowing deeper techniques to be achieved with more ease. This tui na protocol is performed while the patient is supine. First, I begin in the cervical region with finger kneading, thumb pressing and plucking to the posterior cervical muscles, especially at GB 20 and 21. From here, I move to the lateral neck muscles (specifically the scalenes) using finger-kneading and thumb-pushing, plucking at St 11 and 12. When working the scalenes, use care to avoid compressing lymph nodes. Next, I perform grasping and pinching to the SCM at LI 18. Working the SCM for TMJD patients can greatly aid in decreasing headaches, as well as aiding in postural correction too. It is important to not cross the neck of patients to avoid a choking sensation. Be sure to also avoid compression of major circulatory vessels. After the SCM has relaxed, light palpation of the digastrics muscles is indicated at and just lateral to Ren 22. Many TMJD patients who suffer from pain referring into the teeth have great relief when the digastrics are addressed. To properly locate these muscles, the practitioner should have the patient press their tongue against the roof of their mouth. This will cause active contraction of the muscle group. Once all the cervical muscles are released, re-assess joint play, mobilizing any abnormalities discovered.
After the treatment of the cervical muscles, the major muscles of mastication should be addressed. Start with light rubbing and kneading to the temporalis at GB 7 through 9. One-finger pushing to GB 8 is also very effective in opening the local channels. Care should be taken not to overwork these muscles, as the practitioner can induce headaches with improper treatment. Once the local channels have been opened, the massater can be treated with kneading and finger-pressing to Stomach 7 and local ashi points. This area may take some time to release, but it is essential for the last part of the treatment.
Now the superficial jaw muscles have been relaxed and the most important aspect of the treatment can occur; intraoral tui na. The pterygoids (medial and lateral) have the action of grinding, protrusion and lateral motion of the jaw. These muscles are often the most sensitive in treatment of TMJD and require the practitioner to use gloves as a universal precaution. The patient should open their mouth so the practitioner can insert the index finger. It is easiest to use the right hand for the right side and left hand for the left side. Once the index finger is placed in the mouth, it should be moved laterally towards the cheek so the patient can relax their jaw without biting down on the finger. From here, follow the patient's upper teeth to the back of the mouth until a "pocket" is reached. Insert your digit with great care, as being too rapid and aggressive will be very painful for the patient. Once the practitioner has successfully palpated the pterygoids, a constant pressure should be applied within a reasonable comfort level for the patient. Pressing, light kneading and modified plucking can be used, as long as it is done with the patient's pain tolerance in mind. It is important to remember that communication is more difficult with your finger in their mouth. Once the sensation has subsided on one side, the other side can be addressed. Always treat the unaffected side first to gauge the patient's response to this technique.
In my experience, the patient will feel instant relief. I integrate this easy and integrative protocol into my treatment plan for several visits, spacing it out as possible to assure the treatment is working long term. Depending on the length of time the patient has been suffering, anywhere from two to 10 treatments should suffice. Cautions for this treatment include patients that bruise easily, recent oral surgery, and the use of NSAIDs, muscle relaxers or pain killers before treatments. Use lighter pressure in those that bruise easily, and wait until surgical wounds have sufficiently healed so as not to disrupt the healing process. The use of certain medications before treatment can affect sensory perception. This can cause techniques to be too deep, potentially worsening symptoms later.
Finally, when utilizing integrative tui na, it is always important to take your state's scope of practice into consideration. If it is within the legal scope, I highly recommend its integration in treatments of TMJD, as it will greatly decrease the patient's pain, lead to less headaches and allow for a better night's sleep. It also does not add too much time onto your treatments and is very cost-effective especially for the positive results the patient will feel.
Resources
- Zhang E, Ed. Chinese Massage: A Practical English-Chinese Library of Traditional Chinese Medicine. Publishing House of Shanghai University of Traditional Chinese Medicine,1990.
- Xiangcai X. Chinese Tui Na Massage: The Essential Guide to Treating Injuries, Improving Health & Balancing Qi. YMAA Publication Center, 2002.
- Flaws B, Sionneau P. Treatment of Modern Western Medical Diseases With Chinese Medicine, 2nd Ed. Blue Poppy Press, 2001.


